You want dental implants so you can chew with ease and smile with confidence. But implants need a strong base in your jaw to stay secure.
If your bone is too thin or weak, your dentist may suggest bone grafting before moving forward.
You may need bone grafting if you have bone loss from missing teeth, gum disease, or an injury that leaves your jaw unable to firmly support an implant.
When you lose a tooth, the bone in that area can shrink over time. This loss often happens without pain, so you may not notice it on your own.
In the sections ahead, you will learn the clear signs that point to the need for bone grafting for dental implants, how dentists check your jaw, and what the grafting process involves.
With the right information, you can better understand your options and feel prepared for your implant plan.
Key Takeaways
- Dental implants need enough healthy jawbone to stay stable.
- Bone loss from missing teeth or gum disease can necessitate grafting.
- Your dentist uses exams and imaging to determine whether you need additional bone support.
Why Bone Grafting May Be Needed Before Dental Implants
Your dental implant needs solid bone to stay secure for years. If your jawbone has shrunk or weakened, bone grafting can rebuild the support your implant depends on.
The Importance of Jawbone Strength for Implants
A dental implant works like an artificial tooth root. Your dentist places it into your jawbone, where it must bond with the bone through a process called osseointegration.
For this bond to happen, your jawbone must have enough height and width. It also needs good density. If the bone is too thin or soft, the implant may not stay stable while it heals.
After you lose a tooth, the bone in that area begins to shrink. This happens because the jawbone no longer receives stimulation from chewing.
Over time, this bone loss can change how your bite feels and how your face looks.
Experts explain that a dental bone graft can add density and volume to your jawbone. That added strength helps create a stable base for dental implants and supports long-term oral health.
How Bone Loss Affects Implant Success
Bone loss does more than change your jaw shape. It directly affects whether your dental implant can succeed.
If you skip a recommended graft, the implant may not fully fuse with your jawbone. Without strong support, it can loosen or fail.
This risk increases if you have had missing teeth for years or have advanced gum disease.
According to guidance on bone grafting before dental implants, insufficient bone can compromise implant stability and healing.
When the implant cannot integrate properly, you may face added procedures and higher costs.
Common causes of bone loss include:
- Untreated gum disease
- Long-term denture use
- Tooth loss without replacement
- Injury or infection
When you understand how bone loss affects implant success, you can make informed choices before starting treatment.
The Role of Bone Grafting in Implant Placement
Bone grafting rebuilds areas of your jawbone that lack enough structure for an implant. Your dentist places graft material in the weak area, and your body gradually replaces it with natural bone.
This process usually takes several months. During that time, new bone forms and strengthens the site for implant placement.
Many dentists note that a bone graft before implants is necessary for many patients to help prevent complications and improve long-term results.
By restoring lost bone, you improve the chances that osseointegration will occur as planned.
When your jawbone has the right shape and strength, your dental implant can function like a natural tooth.
You gain better stability, improved chewing ability, and stronger support for your overall oral health.
Think you might need bone grafting? Don’t guess, get the facts. Schedule your free dental implant consult today at Total Arch Dental Implant Center in Stuart, FL.
Common Signs You May Need Bone Grafting
Certain changes in your mouth can point to jawbone loss. Missing teeth, gum disease, facial changes, and pain when chewing often signal that your bone may not be strong enough for an implant.
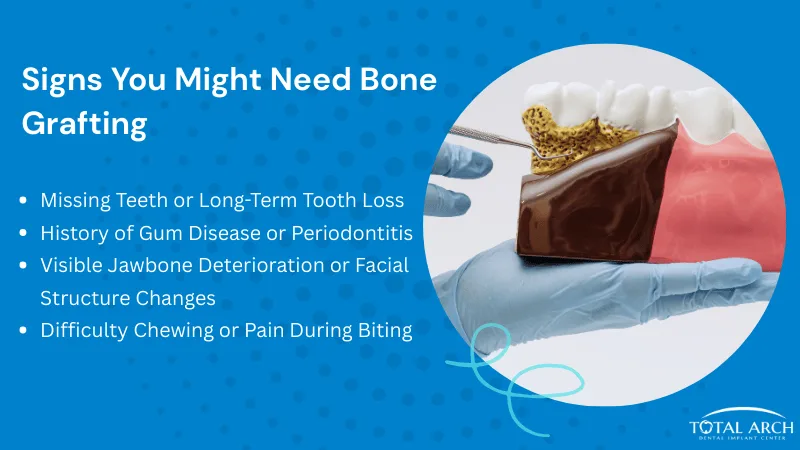
Missing Teeth or Long-Term Tooth Loss
When you lose a tooth, the bone that once held it in place begins to shrink. Your body no longer receives pressure from the tooth root, so it starts to break down the unused bone.
This process can begin within months of tooth loss.
If you have had missing teeth for several years, your jaw may have lost both height and width.
Dentures do not stop this process because they rest on top of your gums and do not stimulate the bone underneath. Many long-term denture wearers develop thinner jawbone over time.
Dentists often see this in patients who delayed treatment after an extraction.
As explained in this guide on 7 signs you may need bone grafting before dental implants, bone shrinkage after tooth loss is common and can affect implant stability.
If your dentist says there is “not enough bone,” bone grafting can rebuild the area and create a stable base for your implant.
History of Gum Disease or Periodontitis
Gum disease does more than cause bleeding gums. In its advanced stage, called periodontitis, it destroys the bone that supports your teeth.
When bacteria spread below the gumline, they damage both soft tissue and bone. Over time, this leads to periodontal bone loss. Teeth may loosen, shift, or even fall out.
Even after you treat the infection, the lost bone does not grow back on its own.
If you have a history of moderate to severe gum disease, your dentist may check your bone levels before placing an implant.
Signs you may need bone grafting before your implant procedure include advanced periodontal disease is a common reason patients need grafting.
Bone grafting can restore support in areas damaged by periodontitis and improve your chances of implant success.
Visible Jawbone Deterioration or Facial Structure Changes
Jawbone loss can change the way your face looks. You may notice that your cheeks appear sunken or that your lips lack support.
These changes occur because bone loss reduces the structural support for your facial muscles. When several teeth are missing, the lower part of your face can appear shorter.
You might also see:
- Loose or shifting teeth
- Gums pulling away from teeth
- Difficulty keeping dentures in place
As described in this article on signs you might need a bone graft before dental implants, visible bone thinning often follows trauma, long-term tooth loss, or gum disease.
If your jawbone has deteriorated, an implant may not anchor securely until the area is rebuilt.
Difficulty Chewing or Pain During Biting
Pain while chewing can signal deeper problems than a simple cavity. When bone loss weakens the support around a tooth, biting pressure can cause discomfort.
You may feel:
- Sharp pain when chewing firm foods
- A dull ache after meals
- Movement in a tooth when you bite down
These signs often appear in areas affected by periodontal disease or untreated tooth loss. Weak bone cannot absorb normal biting forces, which can strain nearby teeth.
Dentists use exams and 3D imaging to measure bone thickness and density.
If they find thin or uneven bone in areas where you plan to get implants, they may recommend grafting to strengthen the site before moving forward.
Diagnostic Methods for Assessing Bone Volume
Your dentist uses imaging and hands-on exams to measure how much healthy jawbone you have. These tests show the exact areas of bone loss and help plan safe implant placement.
Dental X-Rays and 3D Imaging
Dental X-rays give a clear first look at your jawbone. They show bone height, signs of bone loss, and spaces where teeth have been missing.
If you lost a tooth months ago, the image may reveal shrinkage in that area.
Many dentists also use cone beam CT scans. This 3D scan shows bone width, height, and density in detail. It helps your dentist see if the jawbone can hold an implant or if grafting is needed first.
Research shows that visible bone loss on imaging often signals the need for grafting before implant placement.
You can read more about these imaging signs in this guide on signs you may need bone grafting before your implant procedure.
3D imaging also maps nearby structures like nerves and sinuses. This reduces risk and helps your dentist choose the right implant size and position.
Clinical Examination of Jawbone Density
Your dentist also checks your jawbone during a clinical exam. They look at your gums, feel the ridge where the tooth is missing, and check for thin or soft areas.
If the ridge feels narrow or flat, you may not have enough bone width for stable implant placement. A sunken look in your cheeks or jaw can also point to long-term bone loss.
During the exam, your dentist reviews your dental history. Gum disease, long-term tooth loss, and infection often damage the supporting bone.
Even if your gums look healthy now, past disease may have reduced bone density.
By combining imaging with a hands-on exam, your dentist gets a full picture of your jawbone. This careful review guides the decision on whether you need bone grafting before moving forward with implants.
Types of Bone Grafts Used in Dentistry
Dentists use four main types of bone grafts in dental bone grafting: autograft, allograft, xenograft, and synthetic bone graft materials.
Each option rebuilds lost jawbone, but they differ in where the material comes from, how your body responds, and how the surgery is done.
Autograft: Using Your Own Bone
An autograft uses bone taken from your own body. Your dentist or surgeon may remove a small piece of bone from your chin, jaw, or sometimes your hip.
Because the bone comes from you, your body accepts it well. It contains living cells and natural growth factors that help new bone form.
Many dentists consider it a strong option for dental bone grafting when you need solid support for implants.
However, this type of bone graft requires a second surgical site. That means you may have more swelling, longer surgery time, and extra healing. You must be healthy enough for both areas to heal properly.
Autografts often work well for larger defects or when you need significant bone volume before implant placement.
Allograft: Donor Bone Grafts
An allograft uses bone from a human donor. Tissue banks carefully screen and process the bone to make it safe for use.
This option avoids a second surgical site, which can make your procedure shorter and more comfortable.
Your dentist places the donor bone in the area of bone loss, and your body gradually replaces it with your own natural bone.
Allografts are common in dental bone graft procedures, especially for moderate bone loss. They provide a scaffold that supports new bone growth over several months.
You can learn more about how this process works in this overview of a dental bone graft and how it heals.
Healing time varies, but many patients wait three to six months before getting a dental implant.
Xenograft: Animal-Derived Grafts
A xenograft uses bone from an animal, most often cow (bovine) bone. Manufacturers process the material to remove cells and reduce the risk of rejection.
The remaining structure acts as a framework. Your natural bone grows around and into this scaffold over time.
Xenografts are widely used in implant dentistry.
Dentists often choose them for sinus lifts or ridge augmentation, as discussed in this guide on when and why you might need a bone graft before dental implants.
This type of bone graft does not require a second surgical site. Healing may take several months, and some of the graft material can remain in place long term to help maintain volume.
Weak jawbone doesn’t have to mean no implants. Contact us now to learn how bone grafting can rebuild the foundation of your smile. We’ll answer your questions and help you understand every step before you commit.
Synthetic Bone Graft Materials
A synthetic bone graft uses man-made materials, often calcium-based compounds that are safe for the body. These materials are designed to mimic natural bone structure.
Your dentist places the synthetic graft where bone is missing. It supports new bone growth as your body slowly replaces or integrates with the material.
Synthetic options avoid both donor tissue and a second surgical site. That can make them appealing if you prefer not to use human or animal bone.
Different products vary in strength and resorption rate.
Your dentist will choose the material based on how much bone you need, where the graft sits in your jaw, and how soon you plan to place your dental implant.
The Bone Grafting Procedure and Healing Process
Bone grafting for dental implants rebuilds weak or thin jawbone so your implant has a stable base. The process includes placing graft material, protecting the area, and allowing time for new bone to form through osseointegration.

Step-by-Step Bone Grafting Process
Your dentist starts the bone grafting procedure by numbing the area. In some cases, you may receive sedation to help you stay relaxed.
Next, your dentist makes a small cut in the gum to reach the jawbone. They place bone graft material in the area where your bone lacks height or width.
This material may come from your own body, a donor, an animal source, or a synthetic product, as explained in this guide to bone graft materials and procedures.
After placing the graft, your dentist may cover it with a protective membrane. Then they close the gum with stitches.
You go home the same day. Most people return to normal routines within a day or two, but you should avoid hard foods and follow all care instructions to protect your oral health.
Healing Timeline and Osseointegration
Healing takes time because your body must replace the graft with natural bone.
This process usually takes three to six months, depending on the size and location of the graft, as outlined in this overview of bone graft healing before dental implants.
During healing, your body creates new bone cells around the graft. This step supports osseointegration, which means the bone fuses tightly with the future implant.
You may notice mild swelling or soreness for a few days. Your dentist may suggest:
- Soft foods
- Cold compresses
- Avoiding smoking
- Careful brushing near the site
Strong healing supports long-term implant success. Following instructions closely helps protect your oral health and lowers the risk of complications.
Special Considerations for Bone Grafting
Some implant cases require additional steps before placement can succeed. The location of bone loss in your jawbone and your overall health both play a direct role in planning bone grafting.
Sinus Lift and Ridge Augmentation
If you need implants in your upper back teeth, your dentist may suggest a sinus lift. When you lose upper molars, the sinus cavity can expand and reduce the height of your jawbone.
This leaves too little bone for secure implant placement.
During a sinus lift, your surgeon gently raises the sinus membrane and places bone grafting material beneath it. This creates more vertical bone height.
Healing often takes several months before implants can go in.
You may also hear about ridge augmentation. This procedure rebuilds the width or height of a thin jawbone ridge.
Dentists use it when your jawbone has shrunk after long-term tooth loss or gum disease. Ridge augmentation adds graft material to restore the shape and strength needed to hold an implant firmly.
Factors Affecting Eligibility for Bone Grafting
Not everyone qualifies for bone grafting right away. Your dentist will first check the condition of your gums and jawbone.
Active gum disease must be treated before any grafting. Infection can prevent the graft from bonding with your natural bone.
Your medical history also matters. Conditions like osteoporosis or uncontrolled diabetes can slow healing. Smoking reduces blood flow, which lowers the success rate of bone grafting.
Dentists use 3D scans to measure bone height, width, and density. These images help them decide if you need a minor graft, a sinus lift, or a larger ridge augmentation.
If you have been missing teeth for years, your jawbone may have shrunk significantly. In that case, grafting becomes more likely.
You can learn more about common warning signs in this article on the signs you need bone grafting before implants.
Ready to find out if implants are possible for you? Call today to book your consultation to get personalized treatment planning, we’ll guide you through your options with care.
Frequently Asked Questions
You need enough healthy jawbone to hold an implant firmly in place. Dentists look at bone height, width, density, and your dental history before they decide if grafting is necessary.
What indicators suggest a bone graft might be necessary for dental implants?
You may need a graft if you have been missing a tooth for more than six months. The jawbone in that area can shrink without stimulation from a tooth root.
Gum disease is another common reason. It can damage the bone that supports your teeth and leave it too thin or soft for an implant.
If your dentist has told you that you have bone loss on X-rays, that is a strong sign.
How do I know if my jawbone is strong enough for implants without a graft?
You cannot tell by looking in the mirror. Your dentist must check the bone with digital X-rays or a 3D scan.
They measure the height and width of your jawbone where the implant will go. If the bone is thick and tall enough, you may not need a graft.
A clinical exam also helps. Your dentist checks your gums, bite, and any signs of past infection.
Are there any specific symptoms that indicate the need for a bone graft before implants?
Bone loss does not always cause pain. Many people feel normal even when the bone has thinned.
You might notice a sunken look in the gums where a tooth is missing. Some people also see changes in facial shape after long-term tooth loss.
If chewing feels uneven or you avoid one side of your mouth, that can point to bone changes. These signs are discussed in detail in this article on signs you might need a bone graft before dental implants.
What does inadequate bone volume mean in the context of dental implant surgery?
Inadequate bone volume means your jaw lacks the height or width to securely hold an implant. The implant needs solid bone around it to stay stable.
If the bone is too thin, the implant may not bond well. If it is too short, important structures like nerves or sinuses may limit placement.
A bone graft adds volume and density. It creates a stronger base for the implant to attach to over time.
Can bone loss in my jaw be too severe for dental implants, even with grafting?
Severe bone loss can make treatment more complex, but it does not always rule out implants. Your dentist may suggest staged grafting or other techniques to rebuild the area.
In rare cases, the bone may not respond well to grafting. Medical conditions, heavy smoking, or poor healing can affect results.
An in-person exam gives you a clear answer based on your health and bone condition.
How does a dentist determine if a bone graft is required for successful implant placement?
Your dentist starts with a full exam and reviews your medical history. They look for past gum disease, trauma, or long-term tooth loss.
They then take imaging to measure bone density and shape. The dental bone graft process and purpose explain how grafting restores lost bone for implant support.
After reviewing these details, your dentist creates a treatment plan. This plan outlines whether you can place the implant right away or need grafting first.
